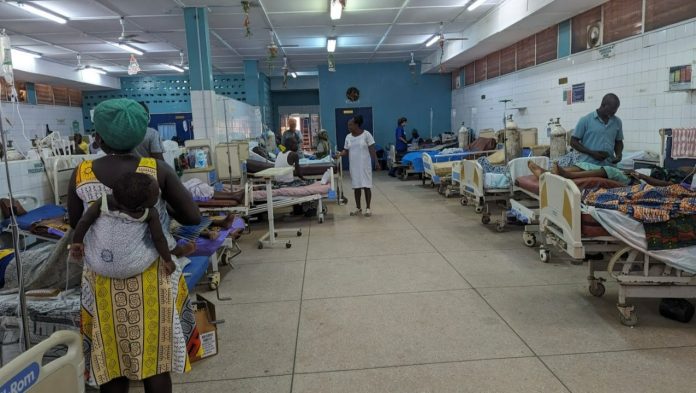
In recent months, Ghana’s health sector has once again come under intense national scrutiny. Persistent challenges in workforce distribution, the picketing of trained professionals demanding placement, and patients forced to receive care on hospital floors all point to a system under severe strain.
The breaking point came with the tragic—and preventable—death of a young man following a road traffic accident, after he was reportedly turned away from multiple hospitals. The incident sparked widespread outrage, drawing the familiar cycle of public anger, media debate, and official pronouncements. The President has reiterated that no patient should ever be denied care, even if treatment must be provided under improvised conditions.
Yet this pattern is not new. It has repeated itself time and again: tragedy, outrage, blame, directives—and then silence. What remains absent is sustained reform. No structural change. It has become so familiar to the point that we have given it a name: “No Bed Syndrome.” But let us be clear, this is not a bed problem. It is a system failure.
The response and why it fails
The Ministry of Health, through its Accident and Emergency guidelines, states that no patient should be denied emergency care because of finance. This aligns with global standards. Through initiatives such as the WHO Global Initiative for Emergency and Essential Surgical Care, countries are encouraged to build systems that prioritise “stabilise first, refer later.”
The problem in Ghana is not the absence of policy.
To its credit, the Ministry of Health responded swiftly in the immediate aftermath of the incident, engaging directly with health facilities to assess conditions on the ground and supplying additional beds to ease congestion. Yet these measures remain short-term interventions that do little to confront deeper systemic weaknesses. Expanding bed capacity alone cannot resolve inefficiencies in patient flow or operational management.
What exists today is a system that absorbs mounting pressure but fails to process it effectively. Too often, responses are reactive—triggered by media outcry or political pressure—resulting in the hurried addition of beds. Meanwhile, patients continue to endure delays of up to 24 hours for basic laboratory results.
Scans are limited to certain hours.
Emergency units remain congested not because beds alone are insufficient, but because patient flow is broken.
We have no structured workflows for overcrowded emergency units.
No alternative care pathways.
No surge protocols.
And in doing so, we place an unfair burden on frontline workers, expecting sacrifice in a system that does not adequately support them. These are professionals already working under extreme conditions, often without sufficient resources, yet bearing the full weight of legal and moral responsibility.
Where the system breaks
The failures are clear: breakdown in prehospital care. Limited coordination and capacity within ambulance services delay critical early interventions. Poor inter-facility communication. No real-time visibility of bed or resource availability. As a result, tertiary centres are overburdened. Facilities such as Korle Bu and 37 Military Hospital receive cases that should be managed at secondary level hospitals.
This is not a failure of individuals.
It is a failure of design.
What we need
Do we really want change?
The answer must be seen in our actions.
If the answer is no, then we can continue responding to crises with statements and short-term optics.
But if the answer is yes, then change requires something far more difficult. It requires long-term, systems-level thinking that outlives political transitions.
Strengthening prehospital services is non-negotiable.
Emergency care must be integrated into national financing and policy frameworks like the NSOAP, to ensure sustainable and measurable improvements in healthcare delivery. A reliable emergency care system requires a coordinated, data-driven network of adequately equipped facilities working closely with frontline providers.
A collective moral responsibility
At its core, the call to strengthening emergency and critical care is not just a technical one, it is also a moral one. No Ghanaian should die because the system could not respond in time. Emergency and critical care should not be a luxury, it is essential, and it reflects how the nation values the lives of its citizens. Every one of us has a role to play, from individuals, management, healthcare workers, private corporations, ministries and agencies.
We must be confident that every Ghanaian, irrespective of position and economic status, will have quality care offered in dignity when needed. We call on the Ghana College of Physicians and Surgeons to consider deliberately integrating leadership and management training into residency programmes through partnership with business schools.
Medical schools can also explore similar options for students who may be interested.
Doctors who eventually end up in management positions in our hospitals must be equipped not only clinically, but also with the skills to effectively lead complex health institutions. There is a clear opportunity for telcos to support emergency care by revamping national referral communication systems and developing a real-time bed management dashboard.
The Ministry of Health Ghana and the Ghana Health Service must collaborate with academic institutions and experts to redesign workflows.
The Ghana Health Service is called upon to institutionalise routine emergency audits.
The National Health Insurance Authority should expand coverage for emergency
care and ensure timely payments to support private sector participation.
The Health Facilities Regulatory Agency can support the categorisation of hospitals into tiers based on capacity and capability, helping to streamline referrals and ensure patients are directed to the right level of care.
Both Parliament and the Ministry of Health have signaled interest in emergency care legislation. Such laws must go beyond punitive measures.
Ghana needs a comprehensive Emergency Care Act with realistic benchmarks, clear timelines and dedicated financing, developed in consultation with key stakeholders.
Emergency care reform is not the responsibility of one institution. It is a coordinated effort across policy, financing, service delivery and accountability working together as a system.
• The writer is Chair, International Student Surgical Network (InciSioN) Ghana and Global Surgery and Health Systems Advocate