Health authorities have renewed focus on the Nipah virus, a rare but highly lethal infectious disease that continues to cause sporadic outbreaks in parts of Asia. Concerns stem from its high fatality rate and the absence of approved treatments or vaccines. Nipah is a zoonotic virus, capable of spreading from animals to humans through contaminated food, and in some cases via person-to-person transmission.
The virus was first detected in 1999 during an outbreak among pig farmers in Malaysia and Singapore, which led to severe illness and significant loss of life.
Fruit bats of the Pteropus genus—commonly known as flying foxes—are recognised as its natural reservoir, shedding the virus through saliva, urine, and droppings. Research has also shown that Nipah can infect other animals, including pigs, dogs, cats, goats, horses, and sheep, which can act as intermediate hosts and heighten the risk of human exposure.
After infection, symptoms usually emerge within four to 21 days, though rare cases with longer incubation periods have been documented. The illness often begins abruptly with fever and flu-like signs, which can progress to pneumonia or other severe respiratory complications. The most serious outcomes are encephalitis or meningitis, typically developing several days after onset and carrying a very high risk of death. Health experts estimate that 40–75% of those infected with Nipah virus do not survive. Survivors may face lasting neurological issues, such as seizures or personality changes, and in rare cases the virus can reactivate months or even years later.

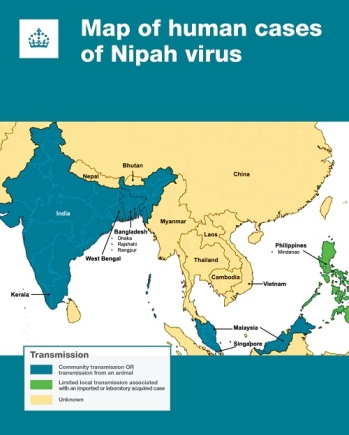
Human outbreaks have been confined to South and South-East Asia, mainly in rural or semi-rural areas. Countries with recorded outbreaks include Bangladesh, where cases have occurred almost annually since 2001; India, with repeated outbreaks in Kerala since 2018 and a current outbreak in West Bengal; as well as Malaysia, Singapore, and the Philippines. Although antibodies to Nipah virus have been found in bats across Asia, Ghana, and Madagascar, no human outbreaks have been reported outside South and South-East Asia.
Transmission to humans often occurs through direct contact with infected animals or by consuming food contaminated by bats. In several outbreaks, infections were linked to the consumption of raw or partially fermented date palm sap, which can be contaminated by bat saliva or excreta. The sap is commonly known as Khejur juice when raw and as Tari or Khajuri Tadi when fermented. Person-to-person transmission has also been documented, particularly among family members and caregivers in close contact with infected patients, especially those with respiratory symptoms.
There is currently no proven treatment for Nipah virus infection and no licensed vaccine to prevent it. Medical care is limited to intensive supportive treatment for severe cases. However, several experimental therapies, including monoclonal antibodies and antiviral drugs, are under development or in early clinical trials. The World Health Organization has classified the Nipah virus as a priority pathogen requiring urgent research and development, citing its high fatality rate and pandemic potential.
In March 2025, the UK Health Security Agency designated Nipah virus as a high-priority pathogen, highlighting the urgent need for investment in diagnostics, treatments and vaccines. UKHSA is also involved in international response efforts through its Public Health Rapid Support Team. In Bangladesh, where outbreaks occur regularly, the team is working with local partners to support education programmes in schools, aimed at teaching children how the virus spreads and how infection can be prevented, with the goal of protecting entire communities.
Health officials say the risk to most travellers remains very low, provided basic precautions are followed. People visiting affected regions are advised to avoid contact with bats and sick animals, refrain from consuming raw date palm sap, practise good hand hygiene and seek medical advice promptly if symptoms develop during or after travel.
Source: GraphicOnline with files from UKHSA

