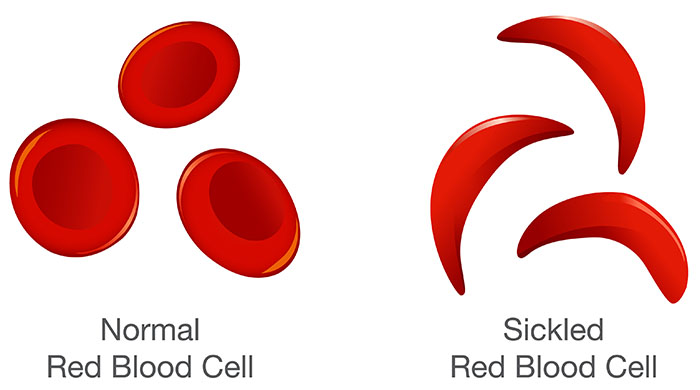
Sickle cell disease (SCD) is a group of inherited disorders affecting red blood cells. Red blood cells are responsible for carrying oxygen throughout the body, using hemoglobin, a protein. In healthy individuals, these cells are round and can easily move through small blood vessels. However, in people with SCD, hemoglobin is abnormal, causing the red blood cells to take on a C-shape, similar to a farm tool known as a sickle. These sickle cells die early, leading to a shortage of red blood cells and a range of complications. When these cells travel through the small blood vessels, they can get stuck and clog the blood flow, leading to pain and other serious health problems such as infection, acute chest syndrome, and stroke.
Types of SCD
People with sickle cell disease (SCD) inherit genes containing abnormal hemoglobin. The type of SCD depends on the specific genes inherited from their parents.
Below are the most common types of SCD:
HbSS
People who have this form of SCD inherit two genes, one from each parent, that code for hemoglobin “S.” Hemoglobin S is an abnormal form of hemoglobin that causes the red cells to become rigid, and sickle-shaped. This is commonly called sickle cell anaemia and is usually the most severe form of the disease.
HbSC
People who have this form of SCD inherit a hemoglobin “S” gene from one parent and a gene for a different type of abnormal hemoglobin called “C” from the other parent. This is usually a milder form of SCD.
HbS beta thalassemia
People who have this form of SCD inherit a hemoglobin “S” gene from one parent and a gene for beta thalassemia, another type of hemoglobin abnormality, from the other parent. There are two types of beta thalassemia: “zero” (HbS beta0) and “plus” (HbS beta+). Those with HbS beta0-thalassemia usually have a severe form of SCD. People with HbS beta+-thalassemia tend to have a milder form of SCD.
SCD is diagnosed with a simple blood test. In children born in the United States, it is most often found at birth during routine newborn screening tests at the hospital. In addition, SCD can be diagnosed while the baby is in the womb. Diagnostic tests before the baby is born, such as chorionic villus sampling and amniocentesis, can check for chromosomal or genetic abnormalities in the baby. Chorionic villus sampling tests a tiny piece of the placenta, called the chorionic villus. Amniocentesis tests a small sample of amniotic fluid surrounding the baby. Because children with SCD are at an increased risk of infection and other health problems, early diagnosis and treatment are important.
Genetic Basis:
Sickle cell disease is primarily caused by a mutation in the HBB gene, which is located on chromosome 11. People who inherit two copies of the mutated gene, one from each parent, will develop SCD. On the other hand, individuals who inherit only one copy of the mutated gene are carriers, often referred to as having sickle cell trait. When red blood cells are exposed to certain conditions, such as low oxygen levels or dehydration, the mutated hemoglobin causes them to change shape and adopt a sickle-like form.
Clinical Manifestations:
The altered shape of sickle cells can impede blood flow, leading to a variety of symptoms and complications. These may include:
Pain Crises: Sudden and severe episodes of pain, known as pain crises, occur when sickle cells block blood vessels, limiting oxygen delivery to tissues.
Anaemia: Sickle cells have a shorter lifespan than normal red blood cells, leading to a chronic shortage of these oxygen-carrying cells and resulting in anaemia.
Organ Damage: The reduced blood flow caused by sickle cells can lead to damage in various organs, including the lungs, kidneys, and spleen.
Infections: Individuals with SCD are more susceptible to infections due to a compromised immune system.
Stroke: The abnormal shape of sickle cells may increase the risk of stroke, especially in children.
Management and Treatment:
While there is no cure for sickle cell disease, several treatment options aim to alleviate symptoms and improve quality of life:
Pain Management: Medications and supportive care are used to manage pain during crises.
Hydroxyurea: This medication can help increase the production of fetal hemoglobin, which reduces sickling.
Blood Transfusions: Regular blood transfusions may be necessary to replace damaged red blood cells.
Bone Marrow Transplant: In severe cases, a bone marrow transplant may offer a potential cure by replacing the patient’s diseased bone marrow with healthy donor marrow.
Public Health Impact:
Sickle cell disease is particularly prevalent in populations with African, Mediterranean, Middle Eastern, and Indian ancestry. It is estimated that millions of people worldwide are affected by this condition. While advancements in medical research and treatment have improved outcomes for individuals with SCD, access to healthcare resources, including genetic counselling and early intervention, remains a challenge in many regions.
Sickle cell disease is a complex genetic disorder that has significant implications for those affected. Continuous research, improved healthcare access, and heightened awareness are crucial for better disease management and enhancing the quality of life for individuals with SCD. As we commemorate another year in the quest to comprehend and treat sickle cell disease, it is essential to continue supporting initiatives that aim to alleviate the burden of this condition on individuals, families, and communities globally.